
Population: 22 hospitalized patients with a diagnosis of acute COPD exacerbation The role of hypoventilation and ventilation-perfusion redistribution in oxygen-induced hypercapnia during acute exacerbations of chronic obstructive pulmonary disease. Hypoxic pulmonary vasoconstriction (Abdo WF 2012)Īubier et al inferred that V/Q mismatch was the primary driver of hypercabia after O2 supplementation, but a follow up study 20 years later looked at it more directly, and their findings muddied the waters. This results in shunting, dead space ventilation, and eventually hypercarbia. Diseased sections of lung see increased PaO2 and steal perfusion away from better functioning areas. Administering supplemental O2 screws up this careful balance. The pulmonary vasculature can dilate and constrict to alter blood flow and match ventilation to perfusion (figure 2), and the primary driver of vascular dilation and increased perfusion is alveolar O2.ĬOPD patients have diseased lungs, and over time their bodies have carefully allocated perfusion to parts of their lungs that work, and away form the parts that don’t. It follows that there must be ANOTHER physiologic change at work, which leads us to… Theory 3: Ventilation Perfusion (V/Q) Mismatch In other words there just wasn’t enough bound CO2 to dislodge. They concluded that the effect, while presumably real, could only have accounted for about 25% of the increase. They calculated how much of the observed change Pa CO2 could be due to the Haldane effect based on the observed change in Hb O2 saturation in their patients. Again we rely on the 1980 Aubier et al study. The chemistry behind this theory is sound, but it’s proved understandably tricky to study in practice. 
This reduces the amount of CO2 that can be bound, and that CO2 winds up dissolved in the blood, resulting in an increased Pa CO2. Supplemental O2 shifts the equilibrium between deoxygenated and oxygenated Hb more towards the oxygenated form. The ability of deoxygenated Hb to bind CO2 is much higher than that of oxygenated Hb (this makes some physiologic sense, because Pa CO2 should be higher in venous blood). The amine groups of proteins in our blood, like hemoglobin (Hb), combine with CO2 to form carbamino compounds. This brings us to a second theory, the Haldane effect. The authors suggested that hypoventilation due to loss of hypoxic respiratory drive WAS NOT the cause of hypercarbia after O2 administration, and that other factors, like the Haldane effect and V/Q mismatching were likely to blame. A follow up study showed that respiratory drive and minute ventilation both stayed within normal limits on supplemental O2. There was NO correlation between minute ventilation and the increase in PaCO2.Ĭonclusions: The study subjects had a transient drop off in minute ventilation on supplemental oxygen therapy, but it did not correlate with steadily increasing PaCO2 levels. At the same time PaCO2 continued to increase (figure 1). Results: All patients had an initial drop in minute ventilation (Ve) once placed on supplemental O2 but Ve then recovered to near baseline levels. Effect of minute ventilation during oxygen-induced hypercapnia. Methods: Minute ventilation and PaCO2 were measured in all patients first while breathing room air and then while breathing supplemental oxygen. Population: 22 ICU patients with known COPD in acute respiratory failure Effects of the administration of O2 on ventilation and blood gases in patients with chronic obstructive pulmonary disease during acute respiratory failure. The first study to really investigate this theory was done in 1980. Supplemental O2 removes a COPD patient’s hypoxic respiratory drive causing hypoventilation with resultant hypercarbia, apnea, and ultimate respiratory failure. Because COPD patients spend their lives chronically hypercarbic they no longer respond to that stimulus, and their only trigger for respiratory drive is the level of oxygen (or lack their of) in their blood. There are two central drivers of respiratory drive, hypercarbia and hypoxemia. One commonly cited theory goes like this: Well lucky for you we sifted through the primary literature to bring you the myths and facts, and the short answer is…it’s complicated. 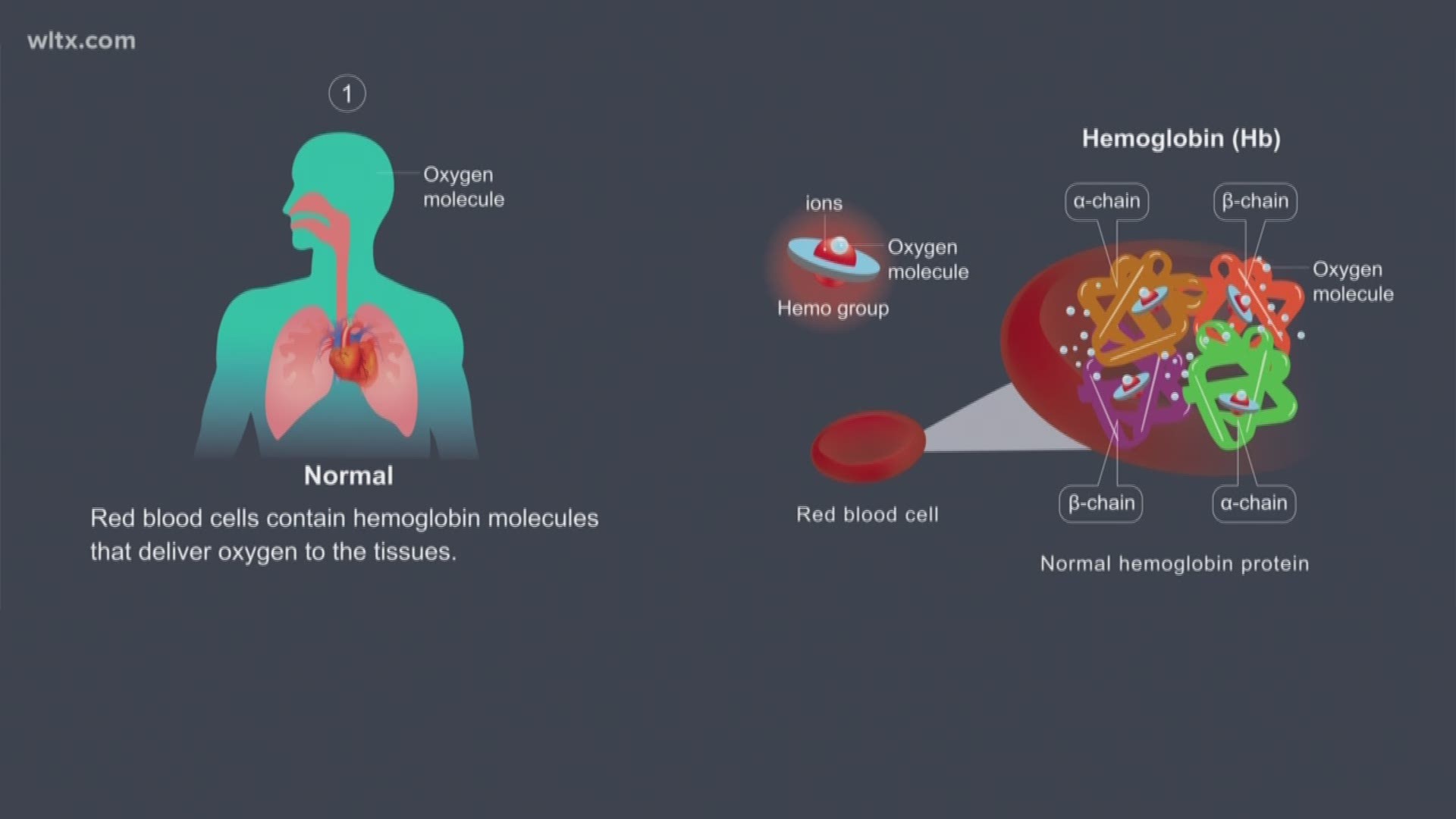
If you’re like me then you’ve probably heard a number of conflicting theories as to WHY overzealous supplemental oxygen leads to bad outcomes in these patients.ĭoes hyperoxia suppress a COPD patient’s respiratory drive? Does it cause V/Q mismatching? Does it change the chemistry of the patient’s blood through the Haldane effect? It’s enough to make you want to give up and page respiratory therapy. We give enough O2 to prevent hypoxemia, but not so much that it causes hypoventilation or dangerous hypercarbia. Background: It’s common practice to give carefully titrated supplemental oxygen therapy for patients in COPD exacerbation.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
